Anemia is described as low levels of hemoglobin in the blood. Hemoglobin is a complex protein that carries oxygen within red blood cells. Without sufficient hemoglobin, our body cannot transport enough oxygen to keep organs and tissues functioning properly.
Unfortunately, diagnosing anemia isn’t as simple as measuring the hemoglobin levels. To determine the underlying cause, several other factors are considered, including:
- MCHC (Mean Corpuscular Hemoglobin Concentration)
- MCV (Mean Corpuscular Volume)
- MCH (Mean Corpuscular Hemoglobin)
- RDW (Red Cell Distribution Width)
MCHC, MCV, MCH, and RDW blood tests help differentiate anemia types, as each requires specific treatment. Comprehensive blood tests not only diagnose anemia but also screen for other blood disorders.
MCHC Blood Test: Mean Corpuscular Hemoglobin Concentration
 Source : Freepik
Source : Freepik
Mean corpuscular hemoglobin concentration, or MCHC blood test, measures hemoglobin concentration in red blood cells relative to their volume. The MCHC blood test isn’t diagnostic for anemia. However, it can help narrow down the possible causes when compared with other blood tests.
The result can be either:
- Low MCHC indicates a low concentration of hemoglobin per red blood cell. It’s often characteristic of iron deficiency, chronic disease, or conditions that affect hemoglobin production.
- High MCHC indicates a higher hemoglobin concentration in each red blood cell. This can occur due to conditions like hereditary spherocytosis, autoimmune disorders, or laboratory artifacts such as hemolysis. Causes include autoimmune disorders, liver disease, sickle cell disease, hypothyroidism, vitamin B12 deficiency, and lymphoma.
The MCHC blood test involves a simple calculation. Multiply the hemoglobin value by 10 and divide by hematocrit (the proportion of whole blood composed of red blood cells).
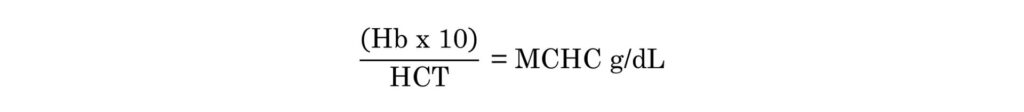
Alternatively, you can simply divide the mean corpuscular hemoglobin (MCH) by the mean corpuscular volume (MCV).
MCV Blood Test: Mean Corpuscular Volume
 Source : Flickr
Source : Flickr
The mean corpuscular volume, or MCV blood test, measures red blood cell size, aiding in anemia diagnosis. Normal adult levels range from 80 to 100 fL.
MCV blood tests define three types of anemia:
- Microcytic anemia (low MCV) is a red blood cell volume under 80 fL. Causes include iron deficiency, chronic disease, thalassemia, sideroblastic anemia, lead poisoning, and spherocytosis.
- Normocytic anemia (normal MCV) is an indicator of hemorrhage, kidney failure, aplastic anemia, leukemia, and bone metastasis.
- Macrocytic anemia (high MCH) occurs in conditions that destroy red blood cells, for example, vitamin B12 deficiency, folate deficiency, liver disease, alcohol use disorder, hypothyroidism, chemotherapy, and much more.
Alongside MCHC and RDW, it can help narrow down the underlying cause. For example, if MCV is high, along with high RDW, it suggests vitamin B12 or folate deficiency. On the other hand, if MCH and MCH are low but RDW is high, then iron deficiency is likely to be the cause.
MCH Blood Test: Mean Corpuscular Hemoglobin
 Source : Freepik
Source : Freepik
The mean corpuscular hemoglobin, or MCH blood test, measures the average hemoglobin content in red blood cells, with normal levels between 27 and 31 pg/cell.
- Low MCH is usually indicative of either low hemoglobin production or red blood cell destruction. Examples include iron deficiency, chronic disease, hemorrhage, kidney disease, liver cirrhosis, and thalassemia.
- High MCH means there is too much hemoglobin within the cell. Causes include vitamin B12 and folate deficiency, leading to megaloblastic macrocytic anemia. It can also occur after living in high altitudes.
RDW Blood Test: Red Cell Distribution Width
 Source : Flickr
Source : Flickr
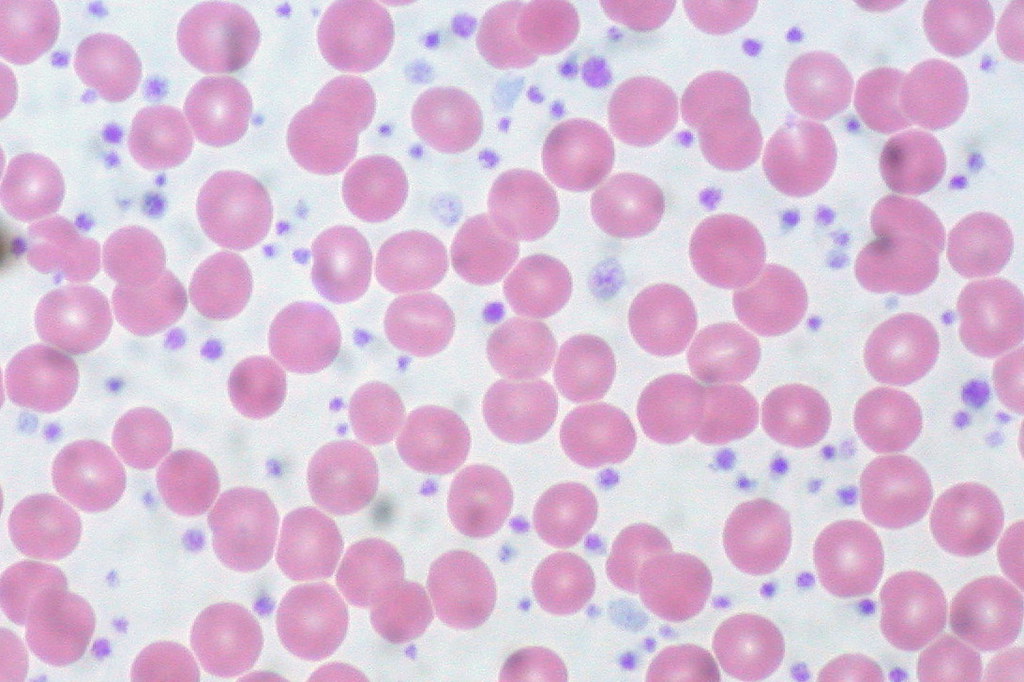
Red cell distribution width, or RDW blood test, evaluates the size variability of red blood cells, with significant variation termed anisocytosis.
- A high RDW blood test indicates a nutritional deficiency. The most common causes include iron deficiency, vitamin B12, and folate deficiency. Other possible causes range from myelofibrosis and chronic inflammation to hereditary conditions like thalassemia and sickle cell anemia.
- Lower RDW indicates uniform red blood cell size, which may be normal in some contexts but needs to be interpreted alongside other indices. Monitoring RDW is crucial to determine if a treatment is working.
How Blood Indices Work Together: Comprehensive Diagnosis
 Source : pexels
Source : pexels
Neither the MCHC blood test nor the RDW blood test is much use alone. It’s only by examining the results collectively that medical professionals can make an accurate diagnosis. Each test helps take the raw diagnosis of anemia and narrow down the possible causes.
For example, a low hemoglobin level could be caused by excessive blood loss (e.g., menstruation), destruction of red blood cells (e.g., chronic inflammation), inadequate hemoglobin production (e.g., iron deficiency), and many more causes. Yet, a glance at the MCHC or MCH would provide an accurate diagnosis or manage the recovery of each condition.
New advanced tools, like NOUL’s miLab™, are speeding up this diagnostic process. Harnessing the power of AI, it allows a faster, more accurate analysis of blood, providing results in just a few minutes.
You might like: CBC Test Normal Ranges: 5 WBC Types and Key Blood Cell Counts
Why Advanced Diagnostics for Blood Indices Matter
 Source : NOUL
Source : NOUL
MCHC, MCV, MCH, and RDW aren’t a random assortment of blood tests. These tests play an essential role in diagnosing nutritional disorders and other hematological conditions. Together, they provide a comprehensive overview of red blood cell size, hemoglobin content, and cell variability.
However, traditional diagnostic methods often come with challenges, such as delays in obtaining results, variability in accuracy across systems, and limited accessibility for smaller healthcare facilities. These limitations can hinder timely and accurate diagnosis.
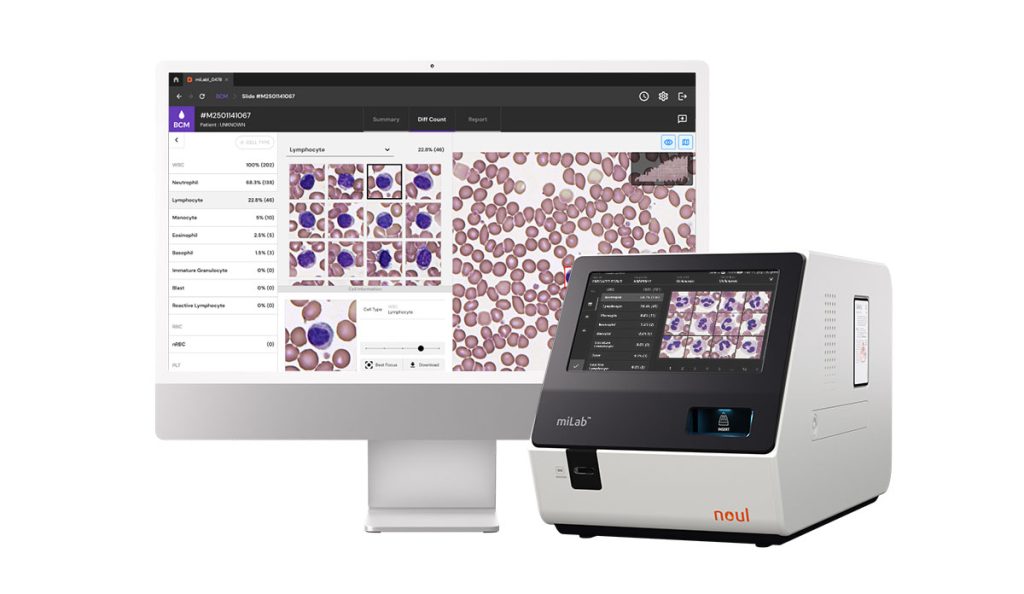
Advanced diagnostic tools like NOUL‘s miLab™ BCM offer rapid and accurate blood analysis, addressing some limitations of traditional systems. The miLab™ BCM provides an average processing time of 20 minutes, ensuring quick results for timely clinical decisions. These point-of-care solutions leverage AI technology to streamline workflows and enhance diagnostic efficiency. Furthermore, the miLab™ BCM integrates NGSI (Automated Smear and Solid Staining) technology, which automates traditionally manual processes, further optimizing workflow and reducing analysis time. In addition to providing a complete blood count (CBC), the miLab™ BCM also includes morphology analysis, offering a deeper insight into the condition of the red blood cells.
Learn more about the power of the miLab™ BCM and explore how it can revolutionize your blood diagnostics. Visit NOUL’s website to discover everything you need to know about the diagnostic platform of the future.

